Surge In Telehealth Appointments, Forced By COVID-19, Spurs New Preference Among People Living With Chronic Conditions
COVID-19 Upended the Patient-Doctor Relationship — For the Better. What Do Consumers Living with Chronic
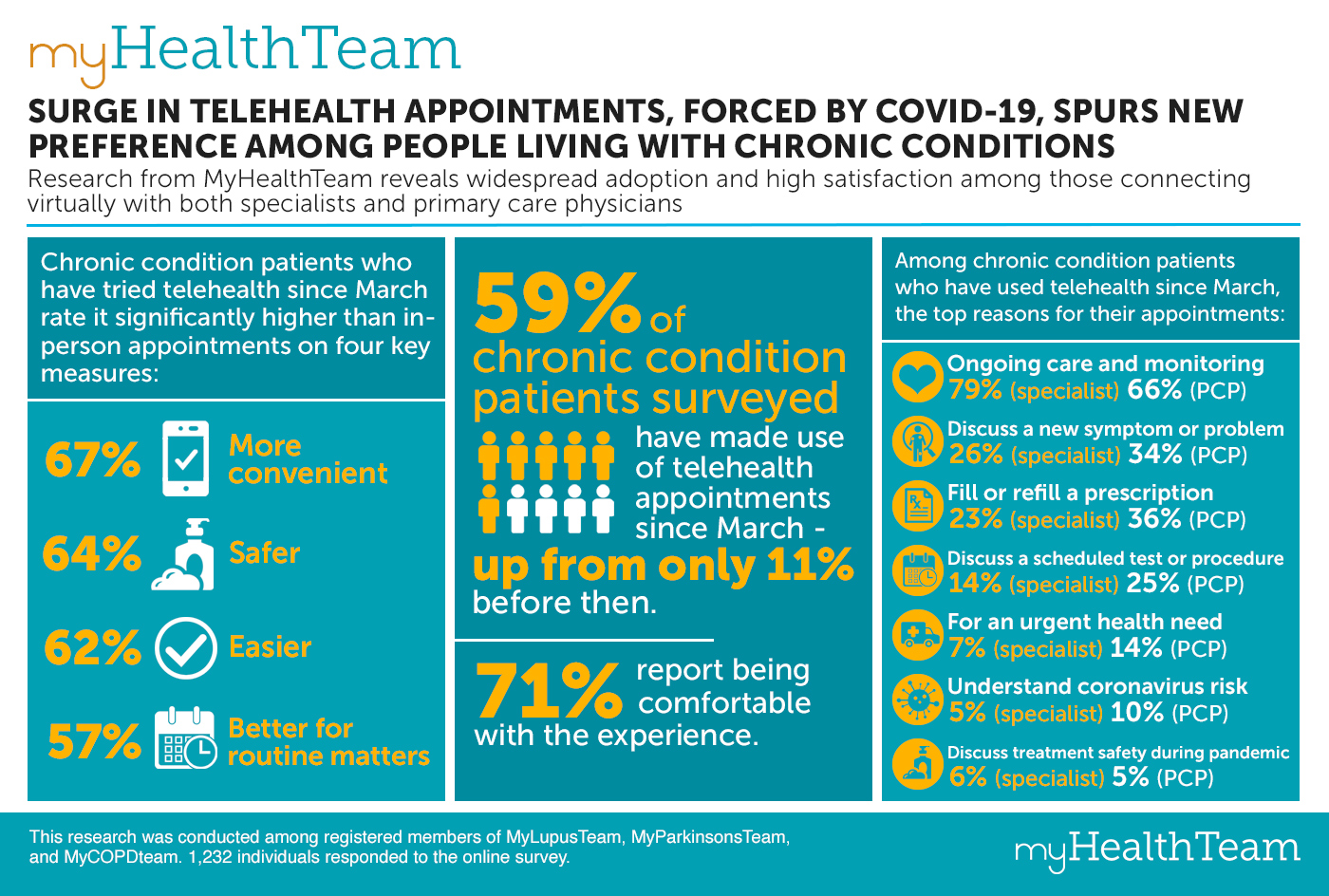
Research from MyHealthTeams reveals widespread adoption and high satisfaction among those connecting virtually with both specialists and primary care physicians
SAN FRANCISCO — August 27, 2020 — Before COVID-19, the commonly held belief about telemedicine was that it would only work for general health concerns (such as fevers, prescription refills, cold and flu) and would not be used by people with chronic conditions and more complex concerns. The coronavirus pandemic forced physicians and their patients to try telemedicine for chronic disease management, creating an opportunity to gauge how it works, why and when it makes sense, and whether patients are likely to use it in a post-pandemic world. MyHealthTeams, creator of the largest and fastest-growing social networks for people facing chronic health conditions, today unveiled new research findings that show people who have tried telehealth since the onset of COVID-19 have a significantly different perception of its value than those who’ve not yet experienced a virtual doctor appointment, and they wish to use it again in the future.
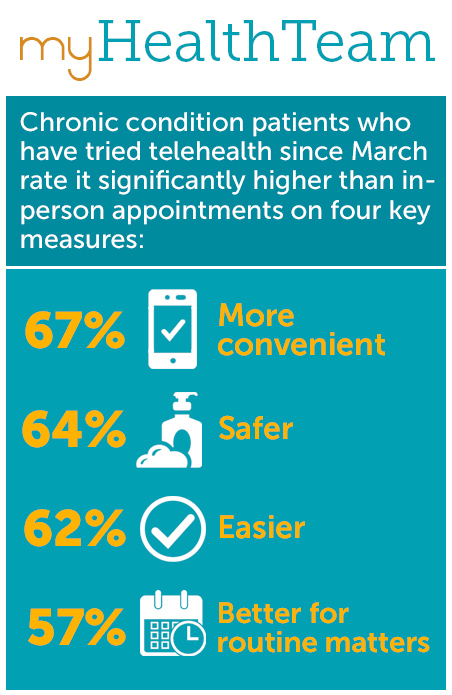
Those who have tried telehealth since March (versus those who have never tried it), rate it significantly higher than in-person appointments on four key measures:
- More convenient – 67% (versus 43%)
- Safer – 64% (versus 41%)
- Easier – 62% (versus 37%)
- Better for routine matters (such as checking in, refilling prescriptions, getting referrals) – 57% (versus 47%)
A majority (57%) of those who have tried telehealth since March say they are likely to use it in the future, post-pandemic – as compared to only 33% of those who have never tried it.
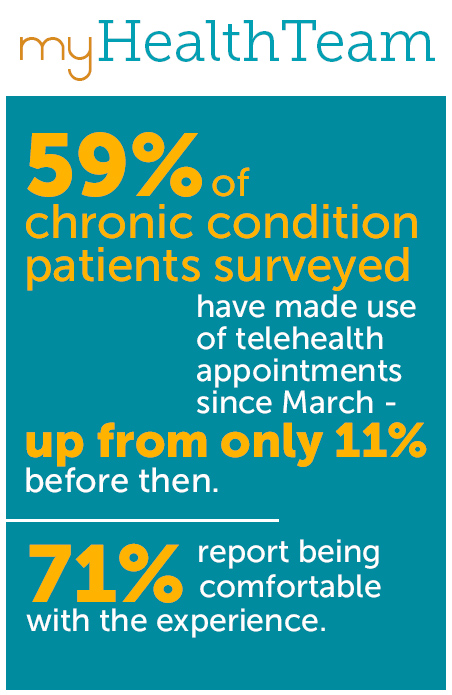
The survey, completed by 1,232 registered members of MyLupusTeam, MyParkinsonsTeam and MyCOPDTeam in July – represented a diverse cross-section of people with chronic conditions facing the difficulty of managing their condition during the coronavirus outbreak. Results showed a huge uptick in telehealth usage, with 59% of those surveyed making use of telehealth appointments since March – up from only 11% before then. Among those who’ve tried telehealth since March, 71% said they were comfortable with the experience.
What Chronic Condition Patients Use Telehealth For: Continuity of Care

Among those surveyed, virtual visits to a specialist (e.g., rheumatologist, neurologist, pulmonologist) slightly outpaced those to a primary care physician (PCP) – with one-third of respondents reporting they’ve seen both via telehealth appointments in the past few months. For both specialist and PCP visits, patients’ reasons for scheduling the appointment reflect a focus on continuity of care and a commitment to maintaining their health during the pandemic. The top reasons cited:
- Ongoing care and monitoring
- 79% of those who’ve “seen” a specialist via telehealth since March
- 66% of those who’ve “seen” a PCP via telehealth since March
- Discuss a new symptom or problem
- 26% specialist
- 34% PCP
- Fill or refill a prescription
- 23% specialist
- 36% PCP
- Discuss a scheduled test or procedure
- 14% specialist
- 25% PCP
- For an urgent health need
- 7% specialist
- 14% PCP
- Understand coronavirus risk
- 5% specialist
- 10% PCP
- Discuss safety of treatments during the pandemic
- 6% specialist
- 5% PCP
“For the one in two Americans living with a chronic health condition, continued engagement with their specialist is essential – diseases such as lupus, Parkinson’s, COPD and so many others do not shelter in place,” said Eric Peacock, cofounder and CEO of MyHealthTeams. “Telemedicine can be quite effective for check-ins with specialists and general continuity of care.”
The satisfaction rate with respondents’ telehealth experience(s) was equally high among those who’ve seen a specialist (71%) and those who’ve seen a PCP (70%).
Even those who have quickly changed their perception of telehealth, however, continue to believe in-person appointments play an important role in ongoing care. Those who have tried telehealth since March (versus those who have never tried it), rate in-person appointments as better than telehealth for:
- More thorough examination – 88% (versus 86%)
- More personal – 62% (versus 75%)
“The sudden necessity to try telehealth has fundamentally changed people’s perceptions about how it could work in chronic disease management,” said Peacock. “This study shows that people who try telehealth generally like it, are comfortable connecting virtually with their doctors, and for some needs, prefer it over an in-person appointment. Their interest in continuing to use telemedicine even after the pandemic suggests telemedicine should play a bigger role in how providers and payers treat chronic conditions in a post-COVID future.”
This research was conducted among registered members of MyLupusTeam, MyParkinsonsTeam and MyCOPDTeam. 1,232 individuals responded to the online survey. Full findings are available at xxx.
About MyHealthTeams
MyHealthTeams believes that if you are diagnosed with a chronic condition, it should be easy to find and connect with others like you. MyHealthTeams creates social networks for people living with a chronic health condition. Millions of people have joined one of the company’s 37 highly engaged communities focusing on the following conditions: Crohn’s and ulcerative colitis, multiple sclerosis, lupus, fibromyalgia, pulmonary hypertension, spondylitis, eczema, myeloma, hyperhidrosis, vitiligo, rheumatoid arthritis, psoriasis, leukemia, lymphoma, irritable bowel syndrome, Parkinson’s, Alzheimer’s, epilepsy, hemophilia, hidradenitis suppurativa, depression, heart disease, type 2 diabetes, myeloproliferative neoplasms, osteoporosis, spinal muscular atrophy, COPD, chronic pain, migraines, narcolepsy, food allergies, obesity, HIV, PCOS, endometriosis, breast cancer and autism. MyHealthTeams’ social networks are available in 13 countries.
Media Contact
Michelle Cox
press@myhealthteams.com
415-823-7574

